Parenting with OCD presents unique challenges, particularly concerning contamination fears and the implications of overprotective parenting. This article explores how a cognitive-first approach, focusing on understanding maladaptive beliefs, leads to improved mental wellbeing for both parents and children. By fostering flexibility in thinking patterns, we can nurture healthier relationships and resilience in family dynamics.
Understanding OCD and Its Impact on Parenting
Understanding OCD and Its Impact on Parenting:
Obsessive-Compulsive Disorder (OCD) presents unique challenges for individuals in various roles, with parenting being one of the most significantly affected by the disorder. Parents with OCD may grapple with persistent and intrusive thoughts, leading to compulsive behaviors aimed at alleviating distress. These obsessions often include common themes such as fears of contamination, which can unfurl into complex and sometimes overprotective parenting behaviors.
Contamination fears, a prevalent compulsion among those with OCD, revolve around the belief that exposure to certain germs, substances, or environments can cause harm. For a parent struggling with these fears, the urge to shield their child from perceived dangers can inadvertently alter the child’s development. For instance, a parent might emphasize strict hygiene protocols, requiring children to wash their hands excessively or avoid outdoor play due to irrational fears of germs. As an example, consider Sarah, a mother with OCD who constantly wipes down her son’s toys and discourages him from playing with other children at the park, fearing he might catch a sickness. While her intentions stem from love and concern, her actions may create an environment where her son grows anxious about germs and risks, impacting his ability to engage confidently with others.
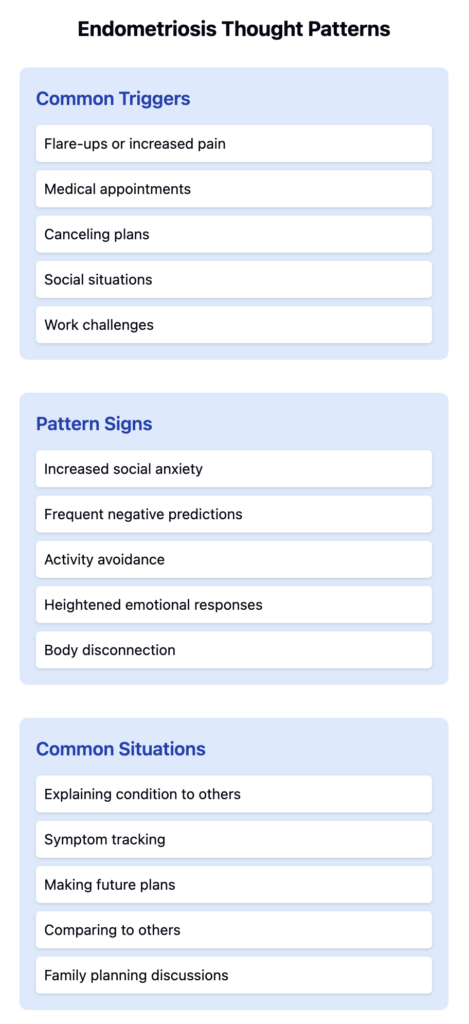
It is essential to understand how the nature of OCD can distort perceptions of everyday activities. Common scenarios such as touching doorknobs or interacting with pets may lead to excessive worry for the parent, forcing them into an overprotective stance. Such behaviors can manifest in children, who may adopt similar anxieties or avoidance strategies. When children witness their parent’s heightened stress around certain activities, they may internalize these fears, creating a cyclical pattern of anxious behavior.
As parents navigate their OCD, it is vital to acknowledge their thoughts and feelings. Acknowledging the irrationality of their fears can be a challenging but essential step toward implementing effective strategies for better coping and fostering a healthier environment for their children. Cognitive Behavioral Therapy (CBT) offers insights that can enable a parent to identify and challenge these thoughts, ultimately leading to healthier parenting practices.
Real-life examples illustrate the importance of creating a balance. For example, Mark, a father dealing with contamination fears, began consulting a therapist to address his OCD. As he learned to challenge and mitigate his irrational fears, he found ways to empower his children by encouraging them to explore activities they previously avoided. This gradual exposure not only helped him lessen his anxiety but also allowed his children to build resilience and confidence.
Recognizing that OCD influences parenting styles significantly can be the foundation for positive change. Understanding the impact of obsessive thoughts on parenting decisions enables parents to foster a nurturing environment while addressing their fears productively. By engaging in therapies and support systems, parents can develop healthier coping mechanisms and improve their children’s emotional well-being, paving the way for an atmosphere of growth and freedom rather than restriction.
The Role of Overprotective Parenting
Overprotective parenting often stems from the desire to shield children from harm, a natural instinct heightened in parents grappling with contamination fears associated with OCD. When a parent, consumed by an ever-present anxiety regarding germs and contaminants, feels compelled to intervene at every turn, this behavior can manifest as hovering or overprotective parenting. The parent may establish strict routines around cleanliness, enforce constant handwashing, and prevent any exposure to situations perceived as dirty or risky. While the intention is to keep children safe, this approach can unwittingly inhibit their development.
Children need opportunities to explore and engage with their environment to cultivate independence and resilience. When a parent is overly vigilant, children may internalize a sense of helplessness and become reliant on their parent’s interventions. For example, a child may become distressed when faced with a natural, everyday scenario involving dirt—such as playing in the backyard—because they have been conditioned to associate these experiences with danger. This can lead to avoidance behaviors, further compounding fears around contamination, and diminishing their confidence in managing minor inconveniences on their own.
The cycle of overprotective parenting not only stifles a child’s independence but also affects their emotional resilience. For instance, a child who is always shielded from perceived threats may struggle when faced with minor social challenges or physical discomforts, as they have not developed the necessary coping skills. They may experience heightened anxiety in new environments, get overwhelmed in social situations, or display avoidance behaviors that keep them from engaging fully with peers and activities that promote personal growth.
Moreover, children emulating the overly cautious behaviors of their OCD-affected parents may develop their own anxieties. A child who witnesses constant hand sanitization may begin to feel that sanitation is not only important but vital for their safety, leading to their own developing contamination fears. In essence, the parent’s extreme protective mechanisms can inadvertently normalize anxiety, establishing a foundation for the child’s own obsessive-compulsive thought processes.
Balanced parenting approaches are essential for fostering emotional health within the family unit. Practical strategies include allowing children to partake in age-appropriate risk-taking activities while providing support rather than control. For example, instead of prohibiting play in the dirt, parents can facilitate discussions about germs, encouraging children to wash their hands afterward while also emphasizing the fun of exploration. Setting clear boundaries around safety without succumbing to excessive control can help children build resilience and self-sufficiency.
Additionally, embracing flexibility in thought and behavior can create a healthier family dynamic. By modeling adaptive responses to perceived threats, parents can teach their children to approach challenges with curiosity rather than fear. Recognizing that some risk is inherent in daily life allows both parents and children to work collaboratively towards developing coping mechanisms, reinforcing the foundation of emotional resilience necessary for navigating life’s unpredictabilities.
Applying CBT for Mental Health in Parenting
Applying CBT for Mental Health in Parenting:
For parents grappling with Obsessive-Compulsive Disorder (OCD), the challenges can be profound, particularly when it comes to managing their own contamination fears while nurturing their children’s development. Cognitive Behavioral Therapy (CBT) offers a structured and flexible approach that can significantly enhance the emotional well-being of both parents and children. By mapping maladaptive beliefs and fostering cognitive flexibility, parents can alter their perspectives and behaviors, ultimately creating a healthier family environment.
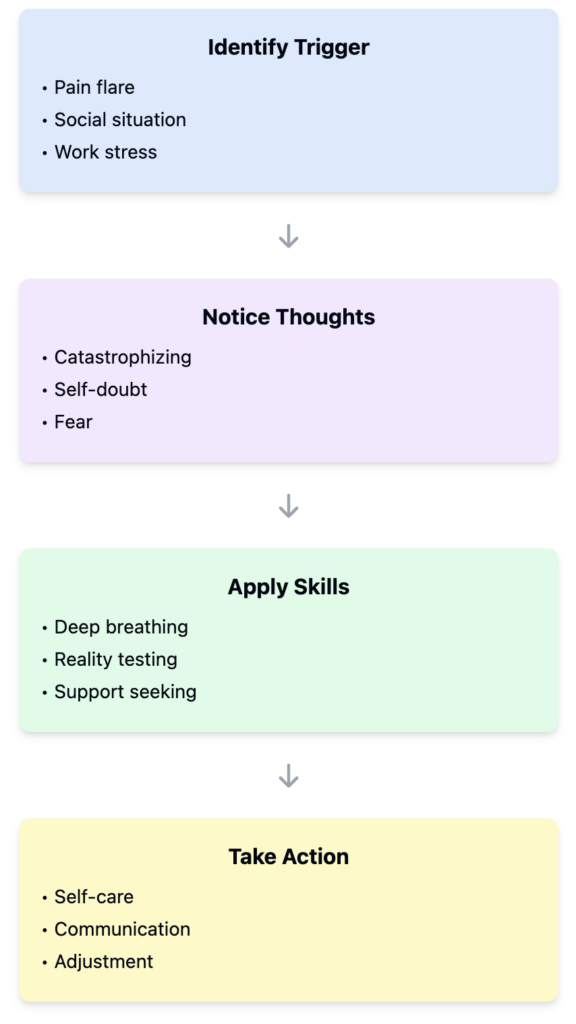
The first step in applying CBT is to identify and challenge maladaptive beliefs. For instance, a parent may hold a belief that all germs pose a serious risk to their child’s health, leading to extreme preventive measures. This hyper-focus on cleanliness and perceived threats can instill fear in children, making them anxious about germs rather than equipping them with healthy coping mechanisms. A practical exercise in CBT involves logging these thoughts when they occur. Parents can keep a thought diary, documenting the situation, their automatic thoughts, and the emotions tied to them.
For example, a parent may encounter a situation where their child touches a public surface and immediately feels the urge to intervene. Instead of reacting immediately, the parent might note their thoughts: “If my child touches that, they will get sick.” Following this, they can challenge it with questions like, “What evidence do I have that this will happen?” or “How do other families cope with similar situations?” This reevaluation encourages a shift from fearful thinking towards more balanced perspectives.
In conjunction with identifying beliefs, developing flexible thinking patterns is crucial. Supportive thinking might include reassurances like, “We can wash our hands after, and that will be sufficient,” while negative thinking may dwell on catastrophic outcomes. Teaching children about safe exploration and the environment fosters their resilience. For instance, a supportive parent might guide their child through an experience, saying, “Let’s touch this and then clean our hands; it’s okay to explore while also being safe.” This not only alleviates the parent’s anxiety but empowers the child.
Furthermore, CBT emphasizes exposure exercises, gradually facing fears in a controlled manner. For example, a parent could intentionally introduce safe, low-level contamination sources into their routine, such as allowing their child to play in sand or engage in art projects without immediate cleaning. Tracking feelings during these exposures can build tolerance over time. As the parent observes their child’s enjoyment and their own discomfort diminishing, it becomes evident that embracing uncertainty can lead to growth.
Moreover, CBT can promote emotional resilience by equipping parents and children with coping strategies. Techniques such as mindfulness, breathing exercises, and positive affirmations can become part of the daily routine. A parent might say, “If I feel anxious, I can take three deep breaths to calm down,” modeling effective coping mechanisms for their child.
By actively applying CBT principles, parents can navigate their OCD challenges more effectively while fostering a supportive, resilient environment for their children. Balancing the understanding of contamination fears with practical, flexible approaches not only enhances symptom management but cultivates a nurturing atmosphere conducive to growth, exploration, and emotional health for the entire family.
Conclusions
In conclusion, parenting with OCD, particularly regarding contamination fears, requires a nuanced understanding of how excessive protection can impact children. By implementing a cognitive-first approach through CBT, parents can transform maladaptive beliefs into supportive thoughts, nurturing resilience in both themselves and their children. Recognizing the interconnectedness of beliefs, thinking, and feelings is essential for fostering a healthier family dynamic.